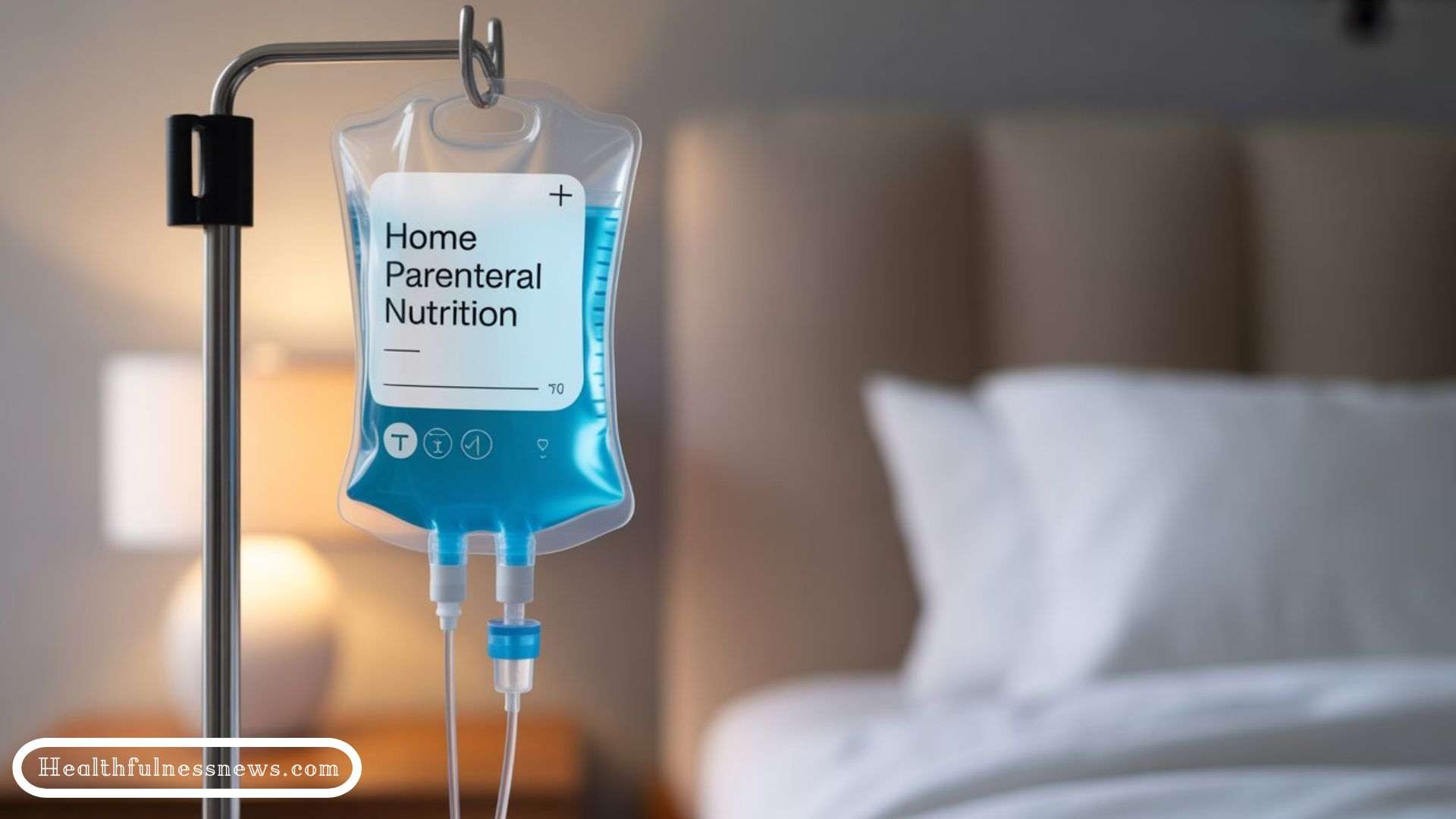
Home Parenteral Nutrition is a way to give your body nutrients through a vein when you can not eat or digest food. It helps you stay strong and healthy while getting care at home.
Stay tuned with us. We’ll soon share more simple and helpful info about Home Parenteral Nutrition. What it is, how it works and how it can help you stay healthy at home.
What Is Home Parenteral Nutrition?
Home Parenteral Nutrition (HPN) is a medical treatment where patients receive nutrients directly into their bloodstream through an intravenous (IV) line bypassing the digestive system completely.
This type of feeding is used when the gastrointestinal tract cannot absorb or tolerate food or fluids effectively.
Who Needs Home Parenteral Nutrition?
HPN is typically recommended for patients with:
- Short bowel syndrome
- Crohn’s disease or ulcerative colitis
- Cancer involving the gastrointestinal tract
- Bowel obstruction or severe malabsorption
- Gastroparesis
- Chronic intestinal pseudo-obstruction
HPN may be temporary or long-term depending on the medical condition.
What is in a Parenteral Nutrition Bag?
The nutrition formula is custom-made by a pharmacist and may include:
| Nutrient Type | Function |
| Carbohydrates (dextrose) | Provide energy |
| Proteins (amino acids) | Maintain muscle and tissue |
| Fats (lipids) | Support energy and cell function |
| Electrolytes | Balance fluids and pH levels |
| Vitamins and Minerals | Prevent deficiencies |
| Water | Maintain hydration |
How Does Home Parenteral Nutrition Work?
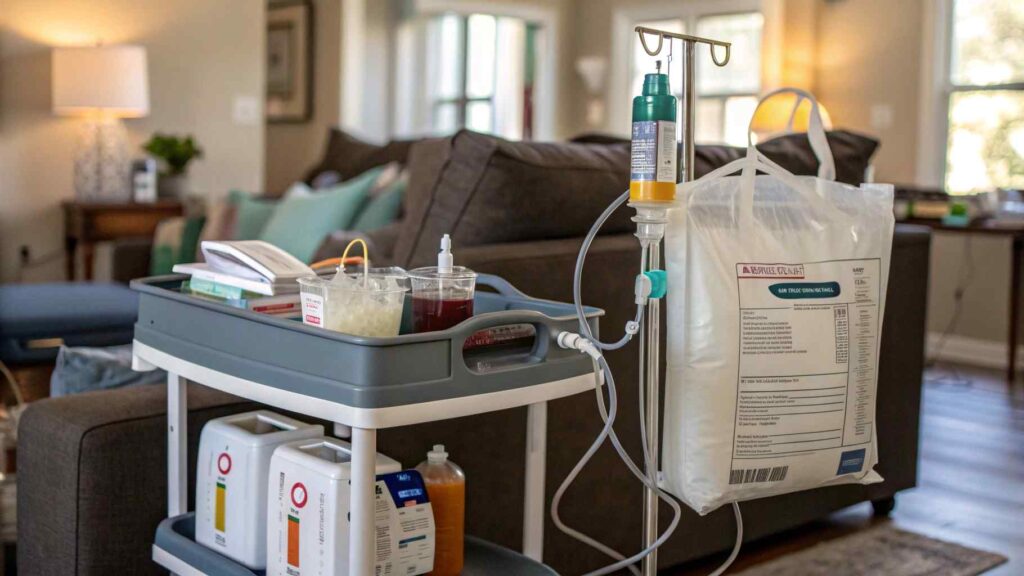
HPN is typically administered through a central venous catheter using an infusion pump:
- Infusion may be cyclic (e.g., 10 to 12 hours overnight)
- A sterile technique is critical to avoid infections
- Patients and caregivers receive training before starting HPN at home
Equipment & Supplies Needed for HPN at Home
- Central venous catheter (PICC, tunneled line or port)
- Infusion pump and IV pole
- Sterile dressings and flushes (saline/heparin)
- Antiseptic solutions
- Pre mixed nutrition bags and tubing sets
- Emergency backup supplies
Steps to Follow for Safe HPN at Home
- Daily Preparation: Wash hands, clean surfaces and set up supplies in a sterile manner.
- Check the Solution: Look for leaks, discoloration or expiration dates.
- Prime the Line: Remove air from the tubing to avoid air embolism.
- Infuse Properly: Use the pump as instructed and monitor for flow rate.
- Monitor for Side Effects: Watch for fever, chills or swelling around the catheter site.
- Flush and Clean: Use saline and heparin flushes as directed to keep the line clear.
A home health nurse often visits regularly to monitor progress and assist with care.
Why Choose Home Parenteral Nutrition? (Advantages)
Home care offers several advantages over hospital based nutrition therapy:
- Improved quality of life and independence
- Reduced hospital stays and costs
- Increased comfort and convenience
- Better long term nutritional management
Patients receive training from healthcare providers to safely manage parenteral nutrition at home.
Common Risks and Complications
While HPN is generally safe, complications can happen. Some of the most common include:
- Infections: Particularly catheter related bloodstream infections (CRBSIs)
- Liver problems: Due to long term fat and carbohydrate infusion
- Blood clots: In or around the catheter
- Electrolyte imbalances
- Dehydration or fluid overload
With proper care most of these issues can be prevented or managed effectively.
How Long Do Patients Stay on Home Parenteral Nutrition?
It varies greatly. Some may need it for a few weeks after surgery, while others with chronic digestive disorders may rely on it for years or even lifelong support. Regular medical check ups are essential to evaluate the need for continued HPN.
Role of the Care Team in HPN
A multidisciplinary team supports the patient at every step:
- Physician (usually a gastroenterologist): Oversees treatment plan
- Dietitian: Customizes nutrient formula
- Nurse: Provides training, catheter care, and infection monitoring
- Pharmacist: Prepares the nutritional solution
- Home infusion company: Supplies equipment and medication
Tips for Living Well with HPN
- Stay organized: Keep a daily log of infusions, weight, temperature and catheter care
- Avoid infections: Follow strict hygiene protocols
- Keep emergency contacts handy: For fever, pain or catheter issues
- Stay hydrated: Drink fluids unless restricted
- Eat when you can: Even small amounts of food (if tolerated) can help stimulate the gut
Can You Travel with HPN?
Yes, with planning! Many patients travel successfully while on home parenteral nutrition. Talk to your healthcare provider in advance to ensure you have:
- Enough supplies
- Backup plans
- A letter from your doctor
- Contact info for emergency care at your destination
Mental and Emotional Support
Living with HPN can be emotionally challenging. It is normal to feel overwhelmed at times. Joining a support group talking with a counselor or connecting with others going through the same journey can be incredibly helpful.
Key Takeaways
| Aspect | Details |
| What is HPN? | Intravenous nutrition delivered at home |
| Who needs it? | Patients with GI issues or nutrient absorption problems |
| Benefits of home use | More comfort, fewer hospital visits, cost savings |
| Key risks | Infection, liver problems, blood clots |
| Support team | Doctors, nurses, dietitians, pharmacists |
| Daily care tips | Hygiene, proper infusion, monitoring signs |
FAQ’s
1. What is home total parenteral nutrition?
Home Total Parenteral Nutrition (TPN) is when a person gets all their nutrients through a vein using an IV at home instead of eating food. It is used when the digestive system does not work properly.
2. What is the procedure for parenteral nutrition?
The procedure involves placing a special tube (catheter) into a large vein usually in the chest or arm. A nutrient rich liquid is then given through this tube using a pump often overnight at home.
3. When to stop parenteral nutrition?
Parenteral nutrition can be stopped when the person’s digestive system is working well enough to absorb nutrients from food or tube feeding. Doctors will decide based on health and lab results.
4. What are the benefits of parenteral nutrition?
Parenteral nutrition helps:
- Provide life saving nutrients
- Maintain weight and strength
- Support healing and recovery
- Improve quality of life when eating is not possible
5. What are the disadvantages of the parenteral route?
Some downsides include:
- Risk of infection from the IV line
- Possible liver problems over time
- It can be costly and time consuming
- Requires careful daily care and monitoring
6. What are the three nutrients to prioritize at each stage of life to optimize physical changes or development?
- Protein: For growth, muscles and healing
- Calcium: For strong bones and teeth
- Iron: For healthy blood and energy
These are especially important during childhood, pregnancy and older age.
Conclusion:
Home Parenteral Nutrition gives people a safe way to get the nutrients they need when eating is not possible. With proper care, support and the right knowledge, patients can live a healthy and active life at home. It truly brings hope, comfort and better quality of life every day.