There is a certain moment — often described by patients as a gradual dimming rather than a sudden change — when cataracts shift from a background nuisance to something that genuinely interferes with daily life. Reading becomes laborious. Night driving feels unsafe. Colors that were once vivid look washed out or yellowed. For older adults navigating this transition, the path from recognizing the problem to understanding the options available can feel far more complicated than the surgery itself typically turns out to be.
Cataracts are among the most common conditions affecting adults over 60, and cataract surgery is one of the most frequently performed procedures in the United States. The procedure itself is refined, the outcomes are generally excellent, and for the majority of patients the recovery is manageable. Yet many people delay seeking evaluation — sometimes for years — because they are uncertain about what treatment involves, what it costs, or whether their insurance will cover it. Getting clear on those questions is often the first real step toward doing something about it.
What Cataracts Actually Do to Vision
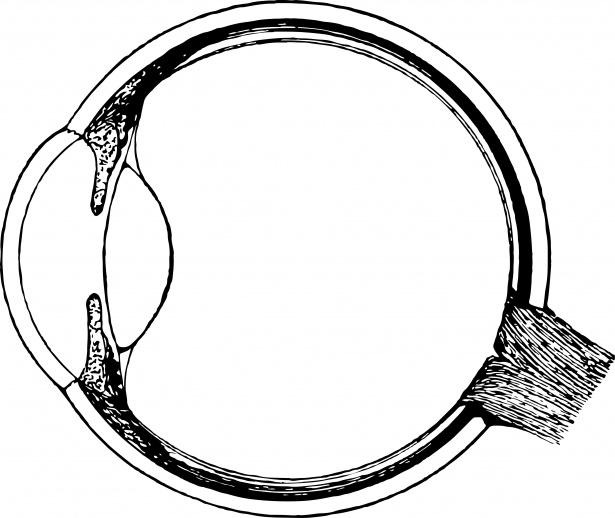
The lens of the eye sits just behind the iris and is normally clear, allowing light to pass through and focus sharply on the retina. Over time, proteins within the lens can begin to clump together and cloud portions of that otherwise transparent structure. The result is a progressive blurring or dimming of vision that glasses alone cannot fully correct, because the problem lies not in how the eye focuses light but in the medium through which light has to travel.
Different types of cataracts affect vision in slightly different ways. Nuclear cataracts, which form at the center of the lens, often cause a temporary improvement in near vision early on — sometimes called “second sight” — before ultimately causing significant blurring and a brownish tint to visual perception. Cortical cataracts, which develop along the outer edges of the lens, tend to create spoke-like opacities that produce glare and light scattering. Posterior subcapsular cataracts form at the back of the lens and are particularly notorious for interfering with reading and causing halos around lights, especially at night. Understanding which type is present can help explain the specific symptoms a patient is experiencing and inform decisions about timing of intervention.
Not every cataract requires immediate surgery. In the early stages, stronger prescription glasses, better lighting, and anti-glare coatings can often compensate adequately. The decision to proceed with surgery is typically based on how much the cataract is affecting quality of life, safety, and independence — not on a fixed threshold of visual acuity alone. That judgment is something best made collaboratively between the patient and their eye care provider.
read more : Vitamin B12 Deficiency: Causes, Symptoms, and Solutions
Understanding Coverage Before Committing to a Plan
For many older adults, one of the first questions after a cataract diagnosis is a practical one: what will this cost, and will Medicare pay for it? The answer is nuanced but generally reassuring. Medicare Part B covers cataract surgery when it is deemed medically necessary, which typically means the cataract has progressed to the point of meaningfully impairing vision and daily function. According to the Medicare coverage information for cataract surgery, the program covers the surgery itself, basic intraocular lens implantation, and one pair of eyeglasses or contact lenses following the procedure — a provision that is specifically unique to cataract surgery among Medicare benefits.
Where costs can increase is in the selection of premium lens options. Standard monofocal intraocular lenses, which restore clear vision at one fixed distance, are covered under Medicare. Patients who want to address astigmatism or reduce their dependence on reading glasses through premium toric or multifocal lenses will typically pay an out-of-pocket upgrade fee, as these represent elective upgrades beyond the medically necessary baseline. The same applies to laser-assisted cataract surgery, which offers precision advantages that some surgeons recommend for specific cases but which is not covered as a standard benefit. Being clear on what Medicare covers — and what falls outside that coverage — allows patients to make informed decisions rather than discovering costs unexpectedly after the fact.
Supplemental Insurance and Out-of-Pocket Considerations
Medicare supplement plans, often called Medigap policies, can offset some of the cost-sharing that remains after Medicare pays its portion — including deductibles and coinsurance amounts. Medicare Advantage plans handle cataract coverage differently depending on the specific plan, so patients enrolled in Advantage plans should confirm their benefits directly rather than assuming they mirror traditional Medicare. For patients managing multiple health conditions alongside their eye care needs, coordinating across providers and insurance plans can become genuinely complex, and having a clear picture of what each plan covers helps avoid gaps in care. Understanding these details ahead of time is worth the effort — particularly for older adults on fixed incomes where unexpected medical costs have disproportionate impact.
Navigating Eye Surgery Resources and Information
One challenge many patients face is simply finding reliable, detailed information about procedures without having to parse through clinical language or sift through content that is more promotional than educational. Eye surgery encompasses a wide enough range of procedures — from cataract removal to corneal transplants to glaucoma interventions — that patients often benefit from having a single, well-organized resource to consult as they move through the evaluation and decision-making process. Platforms like Eye Surgery Today serve that function well, offering procedure-specific content that is accessible without oversimplifying the medical realities patients need to understand.
The ability to go into a surgical consultation already familiar with terminology, procedural steps, and the range of available options changes the dynamic of that conversation. Patients who have done some reading tend to ask better questions, process the surgeon’s recommendations more critically, and leave with a clearer sense of what they have agreed to and why. That kind of informed engagement is not about second-guessing the surgeon — it is about being a more effective participant in decisions that directly affect your own health outcomes.
Recovery at Home and What Support Looks Like
Cataract surgery is an outpatient procedure, and most patients go home the same day, often within a couple of hours of the procedure. For many older adults, that means returning to a home environment without professional medical supervision — which places practical demands on both the patient and whoever is supporting them. The immediate post-operative period involves antibiotic and anti-inflammatory eye drops, activity restrictions, eye shield use during sleep, and avoidance of environments with dust, smoke, or the risk of water exposure near the eye. These are manageable instructions, but they require consistency and some degree of assistance, particularly in the first few days.
For older adults who live alone or whose mobility and dexterity are limited, the logistics of post-operative care are worth thinking through before surgery rather than after. Administering multiple eye drops on a precise schedule is straightforward for some patients and genuinely difficult for others. Arranging for someone to be present during the initial recovery period — whether that is a family member, a neighbor, or a home care professional — reduces the risk of complications that arise from missed drops or inadvertent eye contact. For families navigating home-based care needs more broadly, resources that connect older adults with local support services can be valuable in planning this kind of short-term assistance; a practical overview of Midwest home health care options provides useful context for families in that region thinking through post-surgical support arrangements.
What to Watch for During Recovery
Most patients experience noticeable visual improvement within the first day or two after surgery, though full stabilization of vision can take several weeks as the eye heals and adapts to the new lens. Mild scratchiness, light sensitivity, and occasional blurry periods during the first week are normal. What warrants prompt contact with the surgeon’s office is a different category of symptom: significant pain, sudden vision loss, worsening redness, or the appearance of new floaters or flashes of light. These can indicate complications such as elevated intraocular pressure, infection, or retinal issues that require timely evaluation. Complications are uncommon, but they are best addressed early.
Making the Decision on Your Own Terms
Surgery, even a routine and well-established one, carries weight for patients — particularly older adults who may be managing other health conditions simultaneously or who have limited prior experience with medical procedures. That weight is worth respecting rather than dismissing. The decision to proceed with cataract surgery should feel informed rather than rushed, and patients who feel uncertain should feel entirely entitled to ask more questions, seek a second opinion, or simply take more time before committing.
What tends to shift the calculus for most people is a clear-eyed assessment of what impaired vision is costing them. Reduced independence, heightened fall risk, inability to drive, difficulty reading — these are not trivial inconveniences. For a procedure with a strong safety record, a short recovery window, and meaningful potential to restore functional vision, the barriers to moving forward are often more logistical and informational than medical. Removing those barriers — through better information, earlier conversations with an eye care provider, and practical planning for recovery support — is what makes the whole process feel navigable rather than overwhelming.